Cataract Surgery & Vision Correction
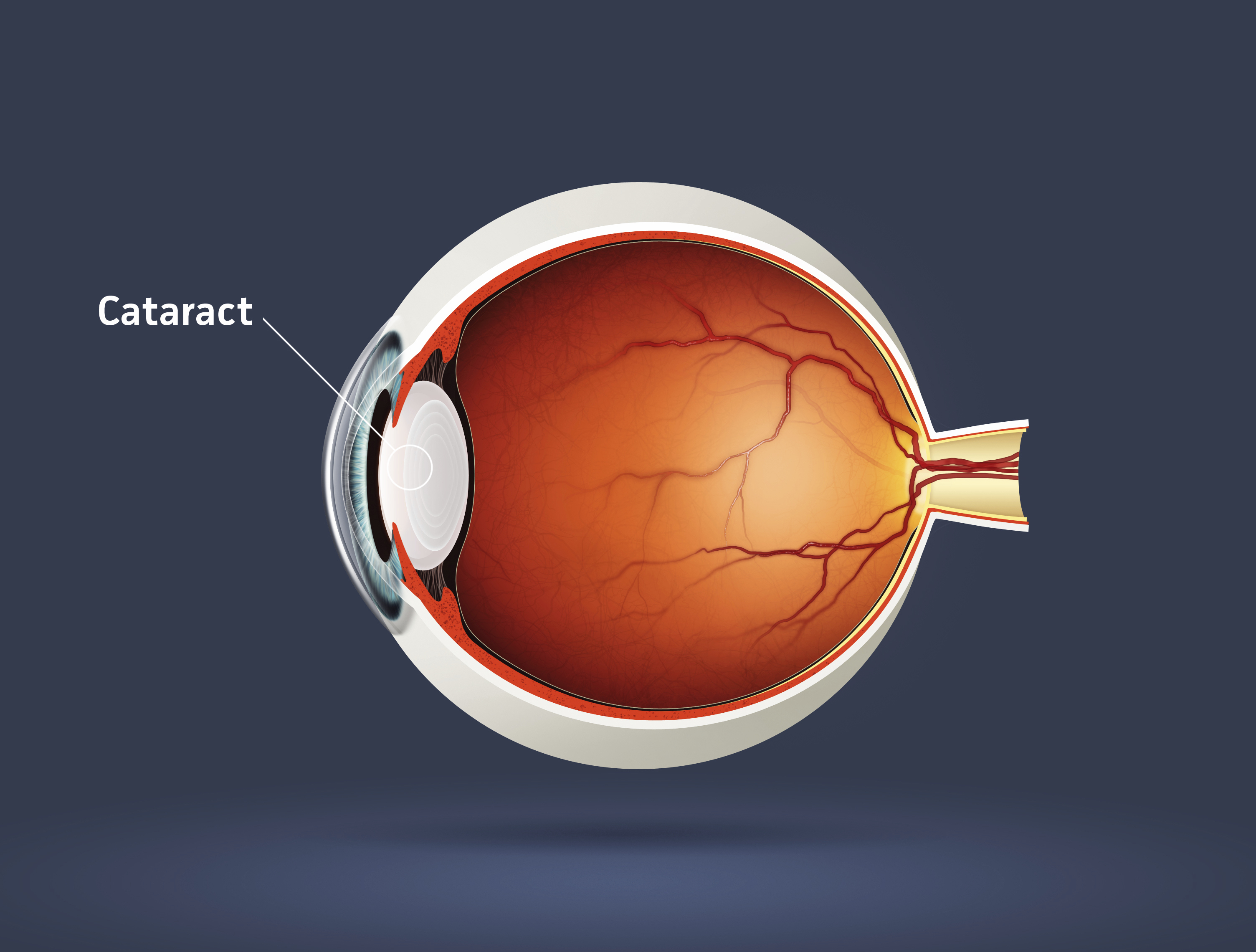
A cataract is a clouding of the normally clear lens of your eye. For people who have cataracts, seeing through cloudy lenses is a bit like looking through a frosty or fogged-up window.
Clouded vision caused by cataracts can make it more difficult to read, drive a car (especially at night) or see the expression on a friend’s face.
Most cataracts develop slowly and don’t disturb your eyesight early on. But with time, cataracts will eventually interfere with your vision.
At first, stronger lighting and eyeglasses can help you deal with cataracts. But if impaired vision interferes with your usual activities, you might need cataract surgery. Fortunately, cataract surgery is generally a safe, effective procedure.
Most cataracts develop when aging or injury changes the tissue that makes up your eye’s lens.
Some cataracts are related to inherited genetic disorders that cause other health problems and increase your risk of cataracts. Cataracts can also be caused by other eye conditions, medical conditions such as diabetes, trauma or past eye surgery. Long-term use of steroid medications, too, can cause cataracts to develop.
How a cataract forms
The lens, where cataracts form, is positioned behind the colored part of your eye (iris). The lens focuses light that passes into your eye, producing clear, sharp images on the retina — the light-sensitive membrane on the back inside wall of your eyeball that functions like the film of a camera.
A cataract scatters the light as it passes through the lens, preventing a sharply defined image from reaching your retina. As a result, your vision becomes blurred.
As you age, the lenses in your eyes become less flexible, less transparent and thicker. Age-related changes cause tissues within the lens to break down and clump together, clouding small areas within the lens. As the cataract continues to develop, the clouding becomes denser and involves a greater part of the lens.
Cataracts may develop in only one eye, but they usually develop in both of your eyes. However, the cataracts usually aren’t totally symmetrical, and the cataract in one eye may be more advanced than the other.
- Cataracts that affect the center of the lens (nuclear cataracts). A nuclear cataract may at first cause you to become more nearsighted or even experience a temporary improvement in your reading vision. But with time, the lens gradually turns more densely yellow and further clouds your vision.
As the cataract slowly progresses, the lens may even turn brown. Advanced yellowing or browning of the lens can lead to difficulty distinguishing between shades of color.
- Cataracts that affect the edges of the lens (cortical cataracts). A cortical cataract begins as whitish, wedge-shaped opacities or streaks on the outer edge of the lens cortex.
As it slowly progresses, the streaks extend to the center and interfere with light passing through the center of the lens. People with cortical cataracts often experience problems with glare.
- Cataracts that affect the back of the lens (posterior subcapsular cataracts). A posterior subcapsular cataract starts as a small, opaque area that usually forms near the back of the lens, right in the path of light on its way to the retina.
A posterior subcapsular cataract often interferes with your reading vision, reduces your vision in bright light, and causes glare or halos around lights at night.
- Cataracts you’re born with (congenital cataracts). Some people are born with cataracts or develop them during childhood. Such cataracts may be the result of the mother having contracted an infection during pregnancy.
These cataracts also may be due to certain conditions, such as myotonic dystrophy, galactosemia, Lowe’s syndrome or rubella. Congenital cataracts don’t always affect vision, but if they do they’re usually removed soon after detection.
Risk Factors
Factors that increase your risk of cataracts include:
- Increasing age
- Diabetes
- Drinking excessive amounts of alcohol
- Excessive exposure to sunlight
- Exposure to ionizing radiation, such as that used in X-rays and cancer radiation therapy
- Family history of cataracts
- High blood pressure
- Obesity
- Previous eye injury or inflammation
- Previous eye surgery
- Prolonged use of corticosteroid medications
- Smoking
Treatment
- The only effective treatment for cataracts is surgery.
- When to consider cataract surgery
Talk with your eye doctor about whether surgery is right for you. Most eye doctors suggest considering cataract surgery when your cataracts begin to affect your quality of life or interfere with your ability to perform normal daily activities, such as reading or driving at night. - It’s up to you and your doctor to decide when cataract surgery is right for you. For most people, there is no rush to remove cataracts because they usually don’t harm the eye.
- Delaying the procedure won’t make it more likely that you won’t recover your vision if you later decide to have cataract surgery. Take time to consider the benefits and risks of cataract surgery with your doctor.
- If you choose not to undergo cataract surgery now, your eye doctor may recommend periodic follow-up exams to see if your cataracts are progressing. How often you’ll see your eye doctor depends on your situation.
- What happens during cataract surgery
Cataract surgery involves removing the clouded lens and replacing it with a clear artificial lens. The artificial lens, called an intraocular lens, is positioned in the same place as your natural lens, and it remains a permanent part of your eye. - For some people, other eye problems prohibit the use of an artificial lens. In these situations, once the cataract is removed, vision may be corrected with eyeglasses or contact lenses.
- Cataract surgery is generally done on an outpatient basis, which means you won’t need to stay in a hospital after the surgery.
- During cataract surgery, your eye doctor uses local anesthesia to numb the area around your eye, but you usually stay awake during the procedure.
- Cataract surgery is generally safe, but it carries a risk of infection and bleeding. Cataract surgery increases the risk of retinal detachment.
- After the procedure, you’ll have some discomfort for a few days. You generally will be healed within eight weeks.
- If you need cataract surgery in both eyes, your doctor will schedule surgery to remove the cataract in the second eye a month or two after the first surgery.
